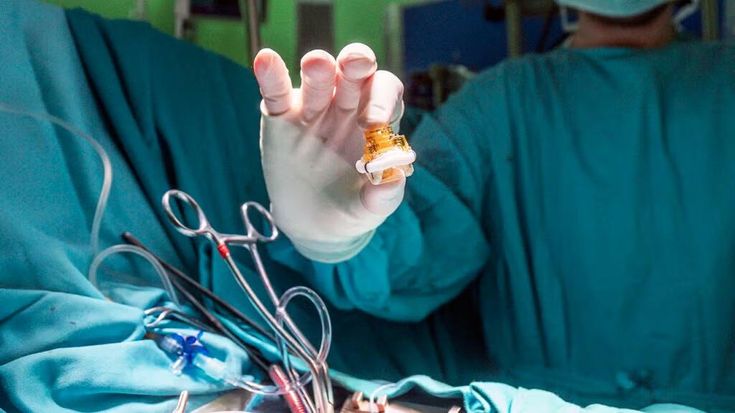
Comprehensive open-heart surgical care for coronary artery disease and valvular heart disease — delivered with precision, experience, and an unwavering commitment to long-term outcomes.
On-Pump CABG is the most widely performed cardiac surgical procedure in the world. It restores blood supply to the heart muscle by surgically bypassing blocked or severely narrowed coronary arteries using conduit vessels (grafts) harvested from elsewhere in the patient’s body.
The operation is performed through a median sternotomy (division of the breastbone) with the patient supported on a cardiopulmonary bypass (CPB) circuit — the heart-lung machine — which takes over the functions of the heart and lungs during surgery. The heart is then arrested using cold cardioplegic solution, providing a still, bloodless operative field in which each graft anastomosis can be constructed with maximum precision.
Once all grafts are completed, the heart is restarted, the patient is weaned from bypass, and the sternum is closed with sternal wires. The procedure typically takes 3–5 hours and constructs 2 to 5 bypass grafts, restoring normal blood flow to all significant areas of diseased coronary territory — a concept known as complete revascularisation.
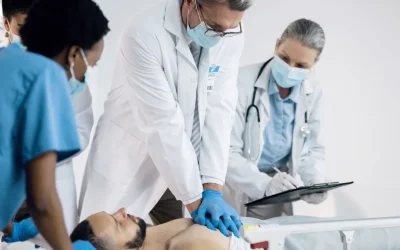
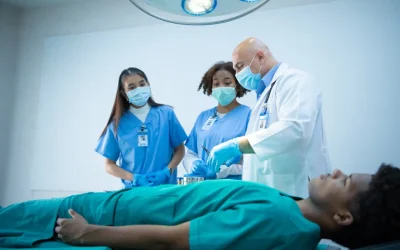

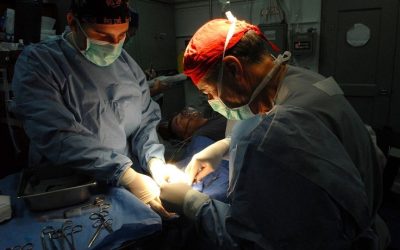
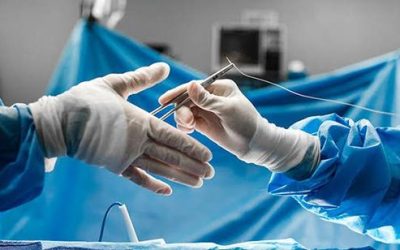
Off-Pump CABG (OPCAB) achieves complete coronary artery bypass grafting through a standard median sternotomy — but without the heart-lung machine (cardiopulmonary bypass circuit). Throughout the procedure, the patient’s heart continues to beat, and each bypass graft is constructed while the target coronary artery is temporarily immobilised using a mechanical tissue stabiliser device (e.g., Octopus, Starfish) applied to the epicardial surface.
By eliminating the bypass circuit, OPCAB avoids the systemic inflammatory response, microembolic load to the brain, haemodilution, and complement activation associated with conventional on-pump surgery. These physiological advantages translate into measurable clinical benefits — particularly in high-risk patient subgroups who are most vulnerable to the side effects of extracorporeal circulation.
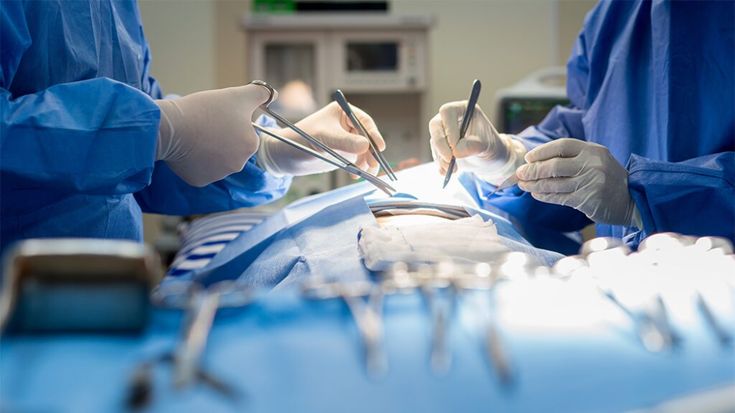
The heart’s four valves — aortic, mitral, tricuspid, and pulmonary — regulate the direction of blood flow through the cardiac chambers. When a valve becomes severely diseased through stenosis (narrowing) or regurgitation (leaking), it places progressive mechanical strain on the heart, ultimately causing heart failure, dangerous arrhythmias, pulmonary hypertension, and premature death if uncorrected.
Dr. Jhulana Jena performs surgical repair and replacement of all four cardiac valves, with particular expertise in mitral valve repair, aortic valve replacement, tricuspid annuloplasty, and combined multi-valve procedures. The operative philosophy is repair whenever feasible — preserving the native valve, its subvalvular apparatus, and the geometric integrity of the left ventricle — to avoid the long-term limitations of prosthetic valves.
Both techniques are safe, and the choice depends on the patient’s condition, number of blockages, and surgeon’s expertise.
The duration varies based on complexity and patient condition.
Yes, surgery is only part of the treatment. Long-term success depends on:
Like any major surgery, risks include:
However, with modern techniques and experienced surgeons, success rates are very high and complications are minimized.
Copyright © 2026 Dr. Jhulana Jena. All Rights Reserved.
Designed With ♥ by Walk Digitally
WhatsApp us